My scoliosis journey, by Margot Messenger
The operation will be worth it, even if you feel a bit low in the days immediately after it. You WILL feel better soon!
I was diagnosed with scoliosis when I was 13 after my family noticed in the summer time that my bikini was sitting wonky on my shoulders and hips.
After being referred to the spinal clinic it was discovered that I had a 40 degree curve. We talked with Mr Upadhyay about the different options…wearing a back brace for most hours of the day, just leaving it and hope it doesn’t worsen or having surgery.
Initially, surgery seemed an extreme option so we just decided to leave it and see how it developed. In the space of a year the curvature had worsened and I was experiencing quite a lot of pain from my back to the point where I was taking ibuprofen for pain relief every day. We decided with Mr Upadhyay that surgery would be the best option for me.
My surgery was scheduled for the end of October in 2018 and I was mentally preparing myself for the operation and missing quite a chunk of school. However that surgery was cancelled because of my poor control over my Type 1 Diabetes, so after preparing myself for the surgery I was quite upset with myself.
The surgery was rescheduled for the summer of 2020 so that I wouldn’t miss out on too much learning for my GCSE exams, so through that year I dealt with the pain of my back and my unhappiness with the way my clothes sat on my shoulders and hips.
Things took a better turn in October of 2019 when blood tests carried out at my routine appointment with my paediatric diabetes team revealed I had achieved really good control over my diabetes. We got in contact with the Bristol spinal team and asked whether my surgery could be moved forward and carried out as soon as possible. We were really lucky there was a slot that Mr Upadhyay could fit me in for surgery the week before Christmas in 2019.
Again, I prepared myself mentally and physically for the surgery, longing to be free of the pain that was bothering me and looking forward to being able to show off my new straight posture in a prom dress the following summer.
The days leading up to the operation were very tense. The hospital was reaching capacity and we knew that operations were being cancelled. There had been a lot of additional arrangements for my surgery as the diabetes and spinal teams had to liaise for my care. This meant that though some routine operations were being postponed, they would pull out every stop to make my operation go ahead. The day we arrived at Bristol Children’s Hospital I was allocated the very last bed in the hospital on a ward that I would come back to after a night in the Intensive Care Unit. With parents in tow, I was taken to the prep room and given my anesthetic and apparently went out laughing.
After waking up post surgery, I was apparently talking about the most random things and even claimed that my favourite band the Arctic Monkeys were in the recovery room with me serenading me! The week following my surgery isn’t very clear in my mind due to the amount of painkillers I was on and the anaesthetic still having an affect on my body. But, I know that only two days after surgery I was learning how to sit up, stand up and walk again after having this massive correction to my spine.
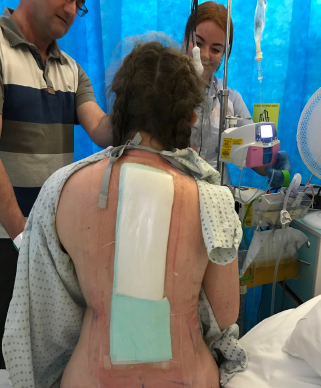
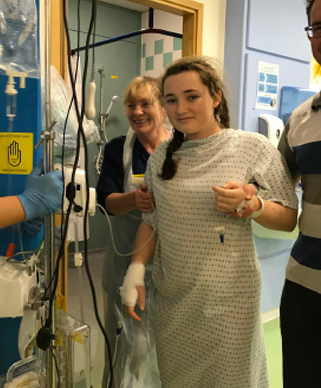

I actually had some minor complications as a result of my diabetes. I’m not going to lie, there were some times when I lay in the hospital bed and wondered if I had made the right decision having the operation. I had quite a few tears and felt pretty miserable. However, the hospital staff were very encouraging. I already wanted to become a nurse, but the wonderful care I was shown inspired me even more. I was cared for by a nurse who had Type 1 Diabetes herself and another who had undergone a scoliosis operation herself at the age of 15. It was great to feel their empathy and I aspire to be able to, one day, offer others the same positivity they gave me. They were always patient, kind and reassuring. Over the next few days, the physiotherapist helped me master going up and down stairs and I gradually improved my movement.
I remember feeling a bit stressed out that I wouldn’t be able to be back home in time for Christmas, but in the end, I was discharged on Christmas Eve. The hour-long car journey home was a little bit painful with all the jolting around over potholes. It was so good to be home! Once home, I needed a lot of support from my family and I honestly don’t really remember a lot from the month of January after my operation. I remember having to be helped in and out of bed and needing support with personal hygiene and not feeling like eating very much.
Gradually, I got stronger and began walking up and down the road. It was the end of January before I felt strong enough to return to school and I did so on a phased return. At first I attended for two hours in the morning, then until lunchtime, then lunchtimes plus the afternoon. By half term, I was able to attend all day, though it tired me out and I had to be very careful not to carry my heavy bag. Luckily I had plenty of friends willing to help. A few weeks later my dreams of wearing my prom dress were crushed as the country went into lockdown. I have kept the dress though and hope that I will soon be able to wear it this summer.
My Top Tips
- Button up nightshirts are the easiest thing to wear while you recover from your operation in the hospital because they can slip over your shoulders easily without lifting your arms and pulling at your wound.
- Make sure your slippers go around your whole foot – the last thing you want is to trip up!
- If you have long hair – tie it up in two plaits. Not only will this keep your hair out of the surgeon’s way, but it will be at least 2 weeks before you can wash your hair and plaits keep it neat.
- Take headphones and an eye mask. It can be noisy and bright at all hours on a children’s ward and it is a relief to be able to zone out with some of your favourite music and darkness. (Good idea for parents too!)
- The meals at the hospital were all really nice, but it is a good idea to have refreshing snacks like grapes and raspberries too. Your parents can keep a few items for you in the parents’ fridge.
Remember
- The operation will be worth it, even if you feel a bit low in the days immediately after the operation. You WILL feel better soon!
- You might feel embarrassed by having to have your parent have to help you out with all the personal stuff. They help because they care. Just accept it, be grateful and move on.
- Build up your walking gradually – try and go a bit further each day.
- Your health is more important than lost school time – don’t stress, you will catch up but you need to recover first.
A parent’s perspective
On our 2016 summer holiday, when we first noticed Margot’s uneven shoulders, we didn’t realise how much her spine would twist and curve over the next three years. I knew that a simple test to bend over and touch the toes would indicate any abnormalities in spine alignment, but was surprised at how uneven her back actually was.
Within two months we had been referred to discuss her condition with Mr Hutchinson and then Mr Upadhyay at Bristol Children’s Hospital. The prospect of surgery was suddenly very real. Margot embraced surgery as a great opportunity to get straightened out, whereas my husband and I feared the consequences that complications could have, especially as, at that stage, Margot’s curve was not particularly noticeable, nor was she in much pain.
However, both the curve and pain grew considerably over the next 12 months and by September 2018, Margot was frequently taking medication to help with back pain. By Summer 2018 we had made a decision to go ahead with surgery in the autumn. Margot was in Year 10 but we felt that an autumn operation would mean that she wouldn’t miss too much school and have plenty of time to catch up before her GCSE Exams in 2020. In addition to her scoliosis, Margot also has Type 1 Diabetes and the impact of this incurable condition would soon become apparent. Pre-op blood checks returned high blood glucose levels and with less than a week to go, the surgery was postponed until such time that Margot had better control of her diabetes with consistently low glucose levels for a number of months. It was just too dangerous to proceed at the time as the risk of infection was much higher.
Margot worked extremely hard to manage her diabetes, and just over a year later, her blood glucose was well-controlled. Her back pain was increasing and after discussions with Mr Upadhyay, it was decided that we could take advantage of this window of opportunity before Christmas to have the operation, allowing plenty of time to recover before sitting her GCSEs.
We went through the pre-op process again, supported every step of the way with excellent communication from and reassurance by the team of professionals involved in Margot’s operation and care. Performance and Operations Manager Ursula Emery, the Spinal Nurse Practitioner Diana Lavelle and Natasha Clark the anaesthetist all liaised with the paediatric diabetes team and provided reassurance. Margot was to go on a sliding scale insulin drip for the duration of the operation and for the day following the operation. After that, my husband and I would take over her diabetes management again.
We spent a tense five hours killing time in Bristol city centre while the operation took place trying to guess when the first cut had been made and what stage the operation had got to. It was such a relief to receive a call from Neil Upadhyay to say that the procedure had been successful and she was waiting for us in the recovery suite.
Even though we had been warned about her appearance, it was still a bit of a shock to see how much her face had puffed up, but we were so relieved that she was through the operation. She was transferred to the ICU for one night and I slept on a fold down bed in the same room. I barely slept, mostly worrying about controlling her diabetes in this totally new situation.
My husband and I spent the next six days relaying between our home in Gloucestershire and the hospital, taking it in turns to stay overnight. For us, the greatest challenge was the management of her diabetes as Margot was too unwell to engage herself with the constant calculations needed to balance carbohydrate and insulin input. The complications Margot experienced with abdominal bloating and fluid on her lung were linked to her diabetes and it was the first time that the spinal team had experienced this reaction, but these issues were resolved within a few days and her recovery was soon back on track.
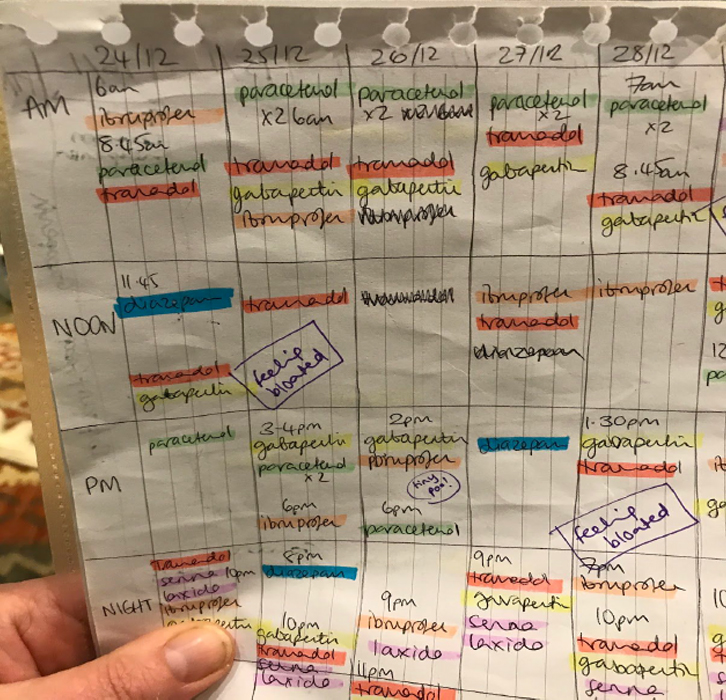
When we left the hospital, we felt rather overwhelmed with the prospect of managing her medication. We drew up a table that helped with keeping track of medication types and administering times. We divided the day into early morning, noon, afternoon and evening sections. This system worked well and mapped out for us when she needed to start easing up on some of the more hard core pain killers.
We were paranoid about her wound becoming infected and followed Diana’s instructions to the letter. Old fashioned sponge washes replaced showers and it was at least three weeks until we washed Margot’s hair. Our first visit to the outpatient clinic ended badly. It was a longer walk than we had anticipated and the combination of Margot feeling exhausted and having taken a tramadol tablet to help with the pain resulted in her passing out in the lobby while we waited for my husband to get the car after the appointment. We then had to wait in A&E for a few hours while they checked her over. In hindsight, we should have pushed Margot to and from the outpatient appointment in a wheelchair.
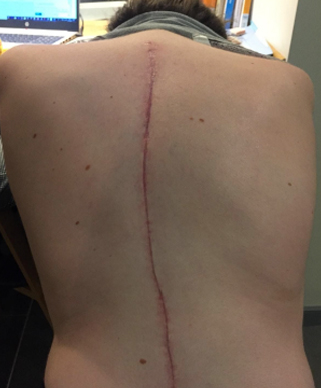
The big reveal once dressings were removed
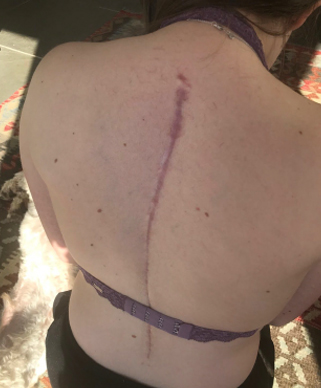
After 6 months
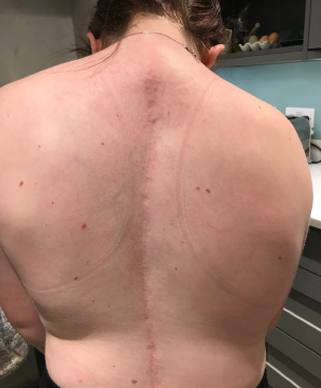
After 12 months
Final thoughts
Though surgery seems a terrifying option when the surgeon details the potential complications and knowing all this, you sign the consent form, it is important to remember that the statistical likelihood of anything going wrong is very low. That’s what I had to keep reminding myself night after night as I lay awake worrying about whether we were making the right decision to proceed with Margot’s surgery.
In Margot’s case, the benefits of having the operation have been extensive. She is now pain free and though her shoulders are not completely level, she doesn’t mind because her back is straight and she has regained confidence in the way she looks. The experience we all had at Bristol Children’s Hospital could not have been better and we were all touched by the care and competency of all of the health care professionals who treated Margot.
Our whole family is hugely grateful to everyone who played a part in looking after her and we feel fortunate to live in a society that benefits from the healthcare that the NHS provides. Margot herself has decided to pursue a career in nursing and this year will be applying to university to begin a nursing degree in September 2022.
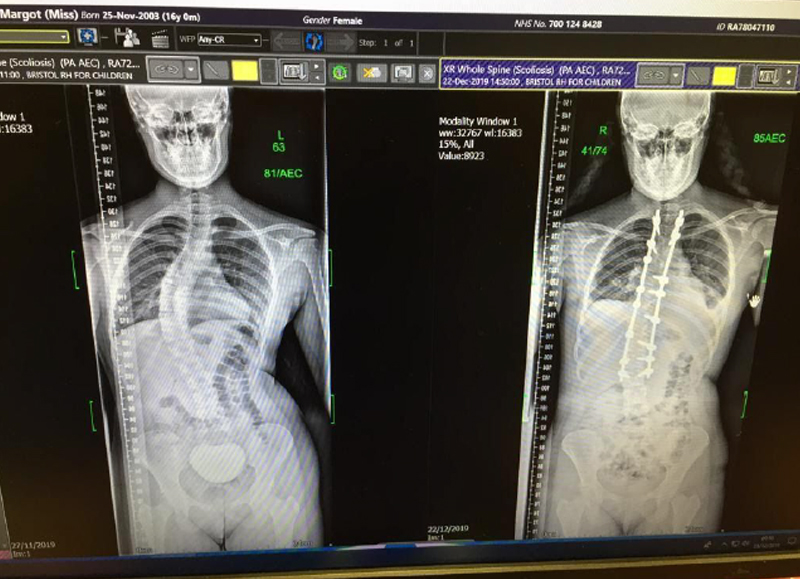
From this… …to this!
